Bacteria are imporant, if not essential, part of a healthy small intestine and fulfill important functions, participate in numerous digestive processes and more. However, overgrowth of small intestinal bacteria can lead to leaky intestinal syndrome and a number of other, often very unpleasant, symptoms. Find out if you also belong to a group of people who can develop SIBO.
Why should you thank the small intestine and the useful bacteria that live in it?
The small intestine plays an important role in the digestion of food and the absorption of nutrients. It is also an important part of the immune system, containing an impressive web of lymphoid cells (cells of the immune system that help fight infections and regulate the immune system).
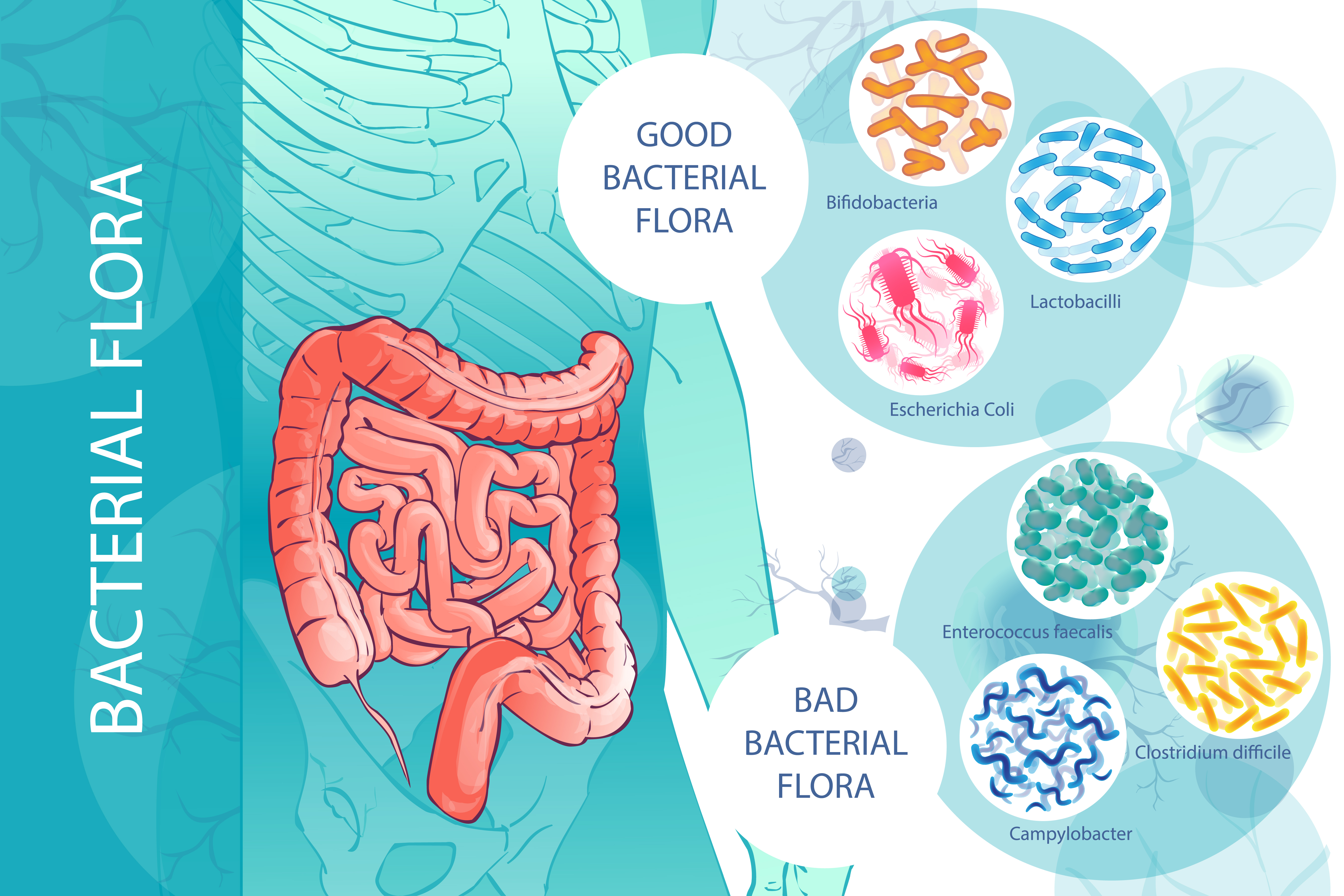
Normal (beneficial, "good") bacteria, which are an important part of healthy small intestine, also fulfill many useful functions. These beneficial microorganisms help to protect against bad (i.e. pathogenic) bacteria and yeasts that are consumed or get into our body in a different way. They help the body absorb nutrients and also produce several nutrients by itself (such as short-chain fatty acids) and vitamins such as folate and vitamin K. These bacteria help maintain normal muscle activity in the small intestine, the so-called peristaltic movements that move the intestinal contents and help to transfer it to other parts of the digestive system.
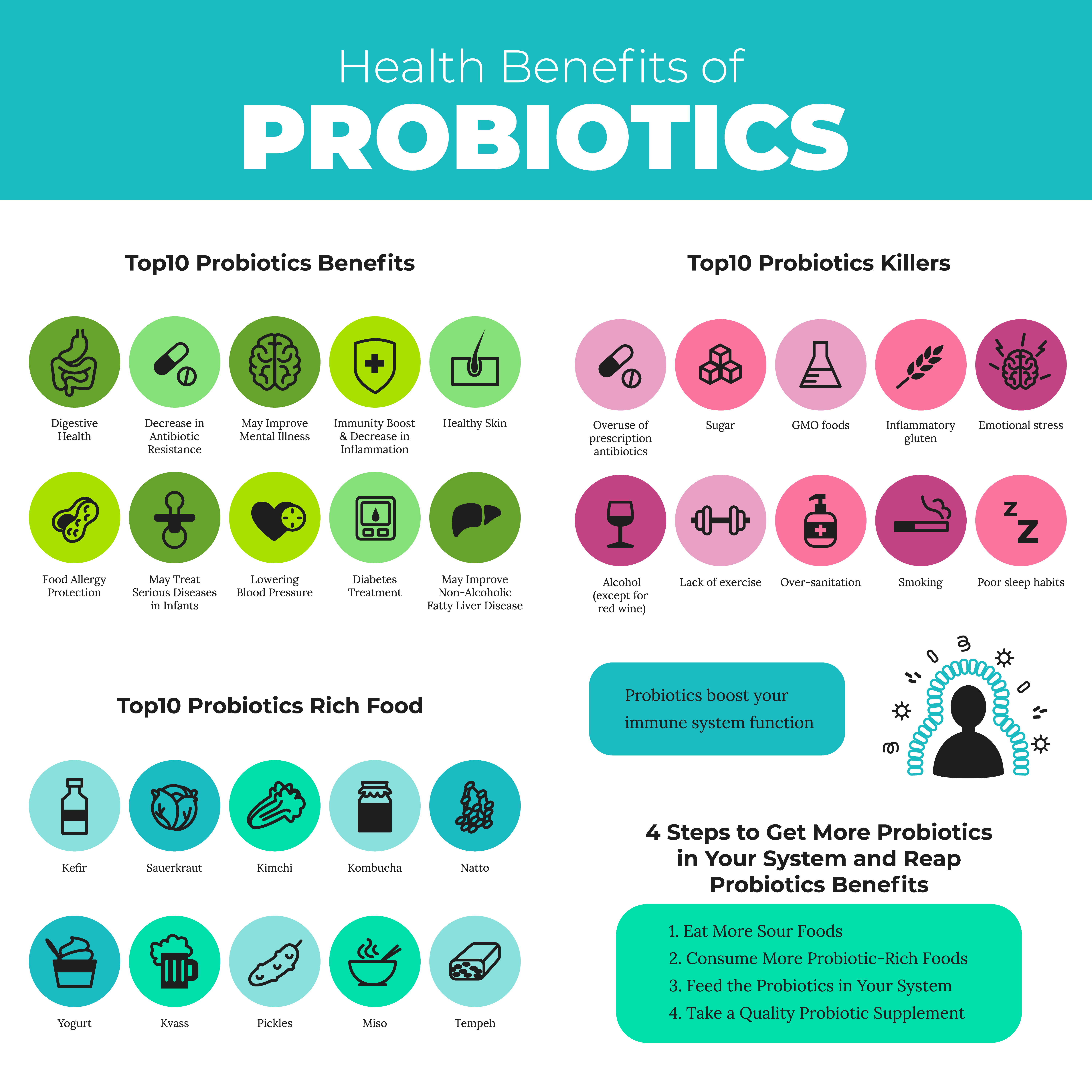
What exactly is SIBO?
SIBO, an overgrowth of small intestinal bacteria, is defined as an increase in the number of bacteria and / or a change in the types of bacteria present in the small intestine. In most patients, SIBO is not caused by a single type of bacteria, but is an overgrowth of the various types of bacteria that normally should occur in the colon (1). Less commonly, SIBO results from the growth of normally occurring bacteria in the small intestine.
It has been shown that SIBO affects both the structure and function of the small intestine. It can significantly affect the digestion of food and the absorption of nutrients, mainly by destroying the cells of the
lining of the small intestine (mucous membrane). In addition, damage to the intestinal mucosa can lead to a leaky guts syndrome (when the intestinal barrier becomes permeable, allowing the large protein molecules to escape into the bloodstream) known to have many potential complications, including immunological reactions that cause food allergies or hypersensitivity, general inflammation and autoimmune diseases (2).
Pathogenic bacteria, regardless of whether they are too numerous or inappropriate, can lead to nutritional deficiencies in the context of insufficient digestion or malabsorption. In particular, bacteria will steal certain B vitamins, such as vitamin B12, before our own cells have the chance to absorb these important nutrients. They may also consume some of the amino acids or proteins that we have absorbed, which can lead to both mild protein deficiency and increased production of ammonia by some bacteria. (Normally, we produce some ammonia from normal proteins and amino acids metabolism, but ammonia needs to be neutralized, so it can additionally burden the detoxification system.) Bacteria can also reduce the absorption of fat through their action on bile acids, leading to a shortage of fat-soluble vitamins such as A and D.
What fosters the development of SIBO?
Our body has several different ways to prevent SIBO. These include gastric acid secretion (maintaining an acidic environment), intestinal muscle waves, intestinal fluid immunoglobulin and a valve that normally allows the contents to flow into the large intestine, but prevents re-inflow back into the small intestine. (This is called ileocecal valve because it is between the ileum and the end of the small intestine with the capsule that forms the first part of the large intestine).
The reason for SIBO is usually complex and probably affects more than one of the above mentioned protection mechanisms. A number of risk factors have been identified for SIBO, and some of the more typical ones are listed below.
Risk factors for SIBO
- Low stomach acid level
- Irritable bowel syndrome
- Celiac disease (long-term)
- Crohn's disease
- Bowel surgery
- Diabetes (type I and type II)
- Many antibiotic therapies
- Internal organ dysfunction, such as liver cirrhosis, chronic pancreatitis or renal failure
Immoderate alcohol consumption and oral contraceptive pills (OCP) also increase the risk of SIBO
Large alcohol consumption has long been associated with the development of SIBO (3). One study also found a relationship between SIBO and moderate alcohol consumption, defined as one drink per day for women and two per day for men. Alcohol appears to affect several normal protective mechanisms, including causing damage to the intestinal mucosa cells, contributing to intestinal leakage and reducing muscle spasms. In addition, alcohol can "graze" several specific types of bacteria, contributing to their excessive growth (4).
In general, there seems to be a moderate relationship between OCP and inflammatory bowel disease (IBD), such as Crohn's disease (5). Although no studies so far correlate the use of OCP with SIBO, given the known relationship between IBD and SIBO, it is likely that this relationship is also true for SIBO. However, when patients stop taking OCP, the risk seems to decrease. .
How to recognize SIBO at home?
The number of people with SIBO in the population remains unknown. Some studies suggest that 6 to 15% of healthy people have SIBO but are asymptomatic. However, as much as 80% of people with IBS may face bacterial overgrowth of the small intestine (6).
SIBO is largely not diagnosed by doctors. This is because many people do not seek support and think that SIBO symptoms are normal digestive problems. Many doctors are not aware of how common SIBO is. The whole matter is further complicated by the fact that the most commonly used tests (breath tests measuring the level of hydrogen and methane) still have quite high rates of false negative results (which means that the test results return as negative, but you actually have the disease) (7).

The most common symptoms of SIBO are:
- Abdominal pain / discomfort
- Flatulence
- Diarrhea
- Constipation (usually associated with methanogens)
- Gases and belching
- In more severe cases weight loss and symptoms associated with vitamin deficiency may occur
Is SIBO contagious?
Unlike many other bacterial infections of the gastrointestinal tract, SIBO is not contagious and there is no evidence that exposure to a single microorganism increases the risk of developing SIBO. SIBO occurs due to the complicated play of many different factors and is not passed between people.
Why is it so hard to recover from SIBO?
Antibiotics are often used to treat SIBO. However, studies show that despite antibiotic treatment, recurrence occurs in almost half of all patients in one year. One study comparing treatment with rifaximin (the most commonly used antibiotic for SIBO) and botanical antimicrobials showed slightly better results in the botanical protocol, but still with successful treatment in almost half of all patients after one treatment cycle.
This finding suggests that treating the growth of bacteria alone is not enough for most people. An additional part of successful treatment must take into account the underlying cause or predisposing factor.
Although there are many identified links between SIBO and other diseases as described above, bowel motility abnormalities are considered one of the most common associations. One of the studies published this month showed that patients with SIBO have significant delays during passage of food in the small intestine (the amount of time required for passage of the small intestine). This finding suggests that patients with SIBO who do not recover after standard antibiotic treatment or the botanical antimicrobial protocol (which we prefer) may benefit from the addition of a prokinetic factor that increases muscle contraction in the small intestine. Octreotide and low-dose naltreotide are two such options that are tested and can help treat some cases of SIBO that do not respond only to antibiotics.
As we continue to study SIBO, we understand better the complexity of the disease and the way in which treatment must be tailored to each individual to maximize success and minimize the risk of relapse.
References
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2890937/
- https://www.ncbi.nlm.nih.gov/pubmed/22109896
- https://www.karger.com/Article/Abstract/201507
- http://onlinelibrary.wiley.com/doi/10.1110/ps.03531404/full
- https://www.ncbi.nlm.nih.gov/pubmed/18684177
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3099351/
- https://www.ncbi.nlm.nih.gov/pubmed/21960820